Snoring is more than a sleep disturbance and a relationship killer for some. It’s a common condition that impacts over 90% of adults and 27% of children at some point in their lives. Though occasional snoring episodes are usually nothing to worry about, persistent or routine snoring is often a serious issue. Sometimes, snoring means there is dysfunction or abnormalities within the internal structures of the nose, mouth, throat, or airways that could lead to severe health complications like sleep apnea without timely medical treatment.
Snoring is a common reason people seek out ENT care. ENT doctors are specialists in ear, nose, and throat disorders. They are best equipped to identify and treat related complications like sinusitis, sleep apnea, nasal congestion, nosebleeds, etc. Though individual patient experiences vary, here’s a brief overview of what happens during a first ENT appointment for snoring.
What Causes Snoring?
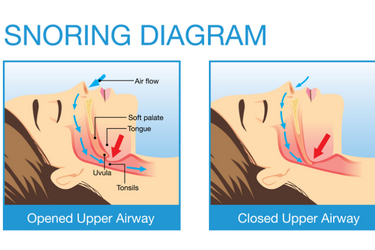
Snoring results from air triggering vibrations in the soft and relaxed tissues of the upper airways during sleep. In some, snoring sounds are soft, and in others, they are loud and disruptive. Some people find they can use nasal strips, nasal irrigation, saline rinses, and decongestants to soften or prevent snoring sounds. But those remedies mask the symptoms and do nothing to address the cause.
First Appointment
In the days leading up to the first ENT appointment for snoring, there are bound to be countless questions and concerns running through your mind about the experience. It’s normal to feel anxious or intimidated at the thought of seeing an ENT doctor for snoring, but there’s nothing to worry about. Here’s why:
You should expect to undergo a physical examination of your mouth, ears, nose, and throat, including often a fiberoptic endoscopy of the nose and throat. Most patients end up snoring from issues that are common with age, lifestyle, health, and other factors. Below are the most common causes of snoring:
Muscle damage, disease, or weakness of the tongue or throat
Aging, alcohol, and some medications cause the muscles in the throat and mouth to become too relaxed and dysfunctional, especially during sleep. Lax muscles can cause the tongue or throat muscles to block the airways.
Swollen throat, mouth, or nasal tissues
Irritants and infections that impact the sensitive tissues in the oral and nasal cavities can cause swelling and inflammation that restricts regular airflow and causes snoring. This is common in children and adults with swollen tonsils, strep throat, colds, allergies, and sinus infections. In rare cases, abnormal tissue growths like polyps or tumors may occur. People who are slightly overweight and obese are at high risk.
Elongated and floppy soft palate or uvula
These long narrow structures in the nasal and throat cavities vibrate during sleep, causing a snoring sound.
Blocked or clogged nasal passages
Nasal congestion is common with upper respiratory ailments and infections, such as asthma, allergies, a common cold, flu or COVID, and sinusitis. But the main difference between sinus congestion and other conditions is sinus related problems never really go away, especially without treatment.
Infection and inflammation are the primary causes of swollen and clogged nasal passages because they prevent proper mucus drainage. Blocked airways also have a higher resistance to airflow that, along with the relaxed muscles due to sleep, create loud, snoring sounds. Snoring activity is often highest during times of the year when allergies flare more frequently or after a bout of infection, such as a cold, the flu, or sinus infection.
Anything that obstructs the nostrils or airways can lead to snoring. Breathing issues and anatomical irregularities in nasal passages are very common. Many people have a deviated septum, nasal polyps, injuries, or structural issues inside their noses that make it harder to breathe easily, comfortably, or adequately, especially during sleep.
The most effective way to correct anatomical nose problems is to see an ENT doctor specializing in snoring treatment for mild to moderate obstructive sleep apnea (OSA). Surgery is often necessary to correct deformities, widen the airways, and stop snoring. Patient weight and snoring severity and additional stipulations may impact treatment options.
What Are ENT Treatments Available for Snoring?
Treatment depends on the cause and the patient’s circumstances. Patients with infections that cause tissue swelling and snoring may benefit from antibiotics, allergy medications, etc. Those who snore because of nasal deformities or swollen or abnormal tonsils or adenoid tissues may require surgery to correct the structures, improve function and airflow, and stop snoring.
Below are the most common ENT treatments for snoring:
Laser assisted uvulplasty (LAUP) with or without soft-palate channeling
This procedure is performed as an in-office procedure. Patients receive local anesthesia to prevent discomfort during treatment. A radiofrequency laser is used to ablate palatal and uvular tissues and stiffen the soft palate to get that loud sound away. Patients go home right away on a soft diet for about 10 days till they see the full effects in 2-3 weeks.
Tonsillectomy/Adenoidectomy
Swollen or infected tonsils and adenoids are a common cause of snoring in both children and adults. Though these structures are less prominent in adults, removing them stops many patients from snoring. Tonsillectomies and adenoidectomies are outpatient procedures. Postoperative patients often experience throat soreness that clears up within the first 1-2 weeks of recovery.
Nasal Surgery
Snoring is a common side effect of nasal congestion, allergies, sinus infections, structural issues, etc. Patients with polyps, a deviated septum, or a collapsed nasal valve can benefit from in-office balloon surgery, inferior turbinate reduction, nasal polypectomy, septoplasty, and endoscopic sinus surgeries. Treatment is based on each patient’s unique circumstances. It is common for some individuals to learn of suitable treatments for their snoring issues during subsequent ENT appointments.
To learn more about ENT treatments for snoring or to schedule your first ENT appointment for snoring, contact C/V ENT Surgical Group.