Common ENT Problems
Ear Tube
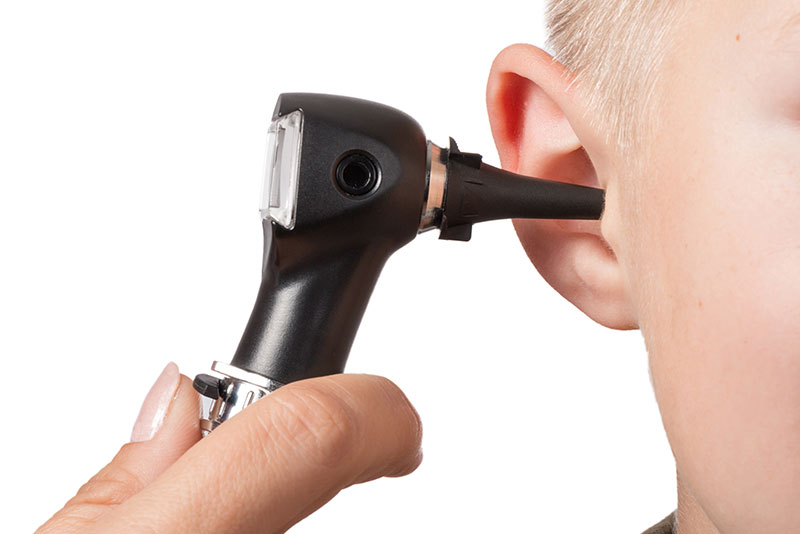
Ear tubes are tiny cylinders placed through the ear drum to allow air into the middle ear. Short- term tubes are smaller and typically stay in place for six months to 2 year before falling out on their own. Long-term tubes are larger and have flanges (T-tubes) that secure them in place for a longer period of time. Long-term tubes may fall out on their own or require removal.
Ear tubes are more common in children for recurrent acute ear infections and/or persistent middle ear fluid with hearing loss. These conditions can occur in teens and adults as well. Other indications for ear tube placement include dysfunction of the eustachian tubes and barotrauma (often seen with changes in altitude with flying or scuba diving.)
Ear tube placement is the most common pediatric procedure performed with anesthesia. In appropriately selected patients, ear tubes can: Reduce risk of future ear infection; resolve hearing loss due to middle ear fluid, improve speech difficulty, and improve behavior and sleep issues.
Myringotomy with insertion of ear tubes is an extremely common and safe procedure with minimal complications. Possible complications include perforation, scarring, infection, and retained or early extrusion of the tube.
- Perforation: A hole in the ear drum may persist after an ear tube comes out. The chance of a persistent hole is higher when a long term tube (T-tube) is used or multiple ear tubes have been placed. The hole can be repaired through a surgical procedure called a tympanoplasty or myringoplasty depending on the size of the hole.
- Scarring: Irritation of the ear drum including recurrent ear infections or repeated insertion of ear tubes can cause scarring of the ear drum. In majority of cases, this causes no problem with hearing.
- Infection: Ear infections can still occur after insertion of ear tubes. These infections are typically less frequent and are easier to treat with ear drops.
- Retained or early extrusion of the tube: Tubes may extrude early with re-accumulation of fluid and need for repeat surgery. Ear tubes may remain too long and result in perforation or require removal.
If you or your child has experienced repeated or severe ear infections, an infection that has not resolved with antibiotics, hearing loss due to fluid in the middle ear, barotrauma, or have eustachian tube dysfunction; our doctors at C/V ENT Surgical Group, serving the greater Los Angeles and San Fernando Valley area, will perform a thorough evaluation and discuss if you or your child is a candidate for ear tubes.
Tonsils and adenoids are part of the immune system. At times, they can become more of a liability than an asset by causing airway obstruction or repeated infections. The tonsils are two masses of tissue that are located in the back of the throat, behind and above the tongue. The tonsils can be visualized in the back of the mouth. The adenoids are located behind the nose and upper throat in between the eustachian tubes. The adenoids are not visible through the mouth or nose without special instruments.

Tonsils and adenoids maybe enlarged without symptoms of tonsillitis. Enlargement of the adenoids may cause difficulty with breathing through the nose, runny nose, and frequent sinus infections. Enlargement of the tonsils and adenoids can cause sleep apnea with loud snoring and gasping for air. Other symptoms include mouth breathing, noisy breathing during the day, and recurrent ear infections. Such obstruction to breathing causes snoring and poor quality sleep that leads to daytime sleepiness, and may even cause behavioral and school issues in some children.
Surgery is reserved for cases of recurrent infections despite antibiotic therapy and/or difficulty with breathing due to the size of tonsils and/or adenoids. Removal of the adenoids maybe indicated in cases of recurrent ear infections or sinusitis in children. In adults, the possibility of cancer or a tumor may be another reason for removing the tonsils and adenoids.
Our specialists at C/V ENT Surgical Group have expertise in treating both pediatric and adult conditions affecting the tonsils and adenoids. They will perform a thorough evaluation and explain both surgical and non-surgical options available based on your specific case.
Tongue-tie (Ankyloglossia)

Indications for treatment depend on age. Infants with tight-tie can have trouble sucking and latching on with resultant poor weight gain. Nursing mothers who experience significant pain while nursing or whose baby has trouble latching on should have their child evaluated for tongue tie. Tongue tie can be an underlying cause of feeding problems and can also lead to abandonment of breast feeding. Toddlers and older children with tongue-tie may have difficulty with articulation of sounds such as “t,” “d,” “z,” “s,” “th,” “n,” and “l.” Children with tongue tie commonly have a V-shaped notch at the tip of the tongue, difficulty with sticking out their tongue, difficulty with touching the roof of the mouth, and difficulty moving the tongue from side to side.
Tongue-tie surgery is a simple procedure. For infants, the procedure may be done in the office. Older children will often require general anesthesia. While frenulectomy is relatively simple, it can yield big results. Our otolaryngologists at C/V ENT Surgical Associates will guide you through the evaluation and determine if your child will benefit from a frenulectomy.
Ear and balance disorders
Cholesteatoma
A cholesteatoma is an abnormal skin growth in the middle ear behind the eardrum. Although a cholesteatoma is not a tumor, it can increase in size and destroy the surrounding delicate bones of the middle ear leading to hearing loss, drainage from the ear, dizziness, and other complications due to injury to the surrounding structures. Repeated infections, a hole in the ear drum, or pulling inward of the eardrum from eustachian tube dysfunction can allow skin into the middle ear and form a cholesteatoma. The eustachian tubes convey air from the back of the nose into the middle ear to equalize ear pressure (ear popping when on a plane or with changes with altitude.)
Individuals with chronic or recurrent drainage from the ears, chronic ear infections, ear pain, hearing loss or dizziness will require an examination by an otolaryngologist. Our doctors at C/V ENT Surgical Group will perform a thorough ear exam and evaluation to determine the presence of a cholesteatoma. Initial treatment may consist of a careful ear cleaning, antibiotics, and ear drops. Initial treatment will aim to stop the drainage. A hearing test and a CT scan maybe performed to determine the hearing level in the ear and the extent of destruction caused by the cholesteatoma. Definitive therapy will usually require surgery. Cholesteatoma is a serious but treatable ear condition, which can be diagnosed only by medical examination. Bone erosion can cause the infection to spread into the surrounding areas, including the inner ear and brain. If untreated, deafness, brain abscess, meningitis, and, rarely, death can occur.
Dizziness and Vertigo
Dizziness can be described in many ways. Vertigo is a specific type of dizziness. Vertigo is a false feeling of motion with sensation as if you or the room is spinning. Some experience dizziness in the form of motion sickness described as a nauseating feeling brought on by the motion. Dizziness, vertigo, and motion sickness all relate to the sense of balance and equilibrium. Your sense of balance is maintained by a complex interaction between different systems in the body including the inner ear, the eyes, the pressure and sensory receptors in the joints, and the brain. The symptoms of motion sickness and dizziness appear when the brain receives conflicting messages from the other systems.
The sensation of vertigo is usually due to an issue with the inner ear. A vertigo attack may cause sudden nausea, vomiting and heavy sweating. Severe vertigo causes a loss of balance and can cause you to fall. During vertigo, small head movements and changes in body position will often make the symptoms worse. An episode of vertigo may last seconds, minutes or hours. Once you are over the first episode, it may never return. However, sometimes symptoms may recur off and on over several weeks or longer, depending on the cause. There may be ringing in the ears or hearing loss, which may be temporary or permanent.
Common causes of vertigo include: Benign Positional Vertigo, Meniere’s disease, migraine, infection, injury, and allergy.
Our experts at C/V ENT Surgical Associated will obtain a thorough history and examination and guide the treatment of your vertigo. A hearing test is often required to evaluate the function of the ear. Treatment will depend on the likely cause of your dizziness.
Middle Ear Infection
Hearing Loss
A conductive hearing loss occurs when sound waves do not reach the inner ear. Sound waves may be disrupted before they reach the inner ear due to a variety of conditions. The ear canal can be blocked by wax, infection, a tumor, or a foreign object. The eardrum can be injured or infected. Abnormal bone growth, infection, or tumors in the middle ear can block sound waves.
A sensorineural hearing loss occurs when sound waves are not processed correctly by the inner ear, the 8th cranial nerve, or central nervous system.
Our specialists at C/V ENT Surgical Group will perform a thorough examination to determine the type and cause of your hearing loss and discuss treatment accordingly.
Hyperacusis
Many people experience sensitivity to sound, but true hyperacusis is rare, affecting approximately one in 50,000 individuals. The disorder can affect people of all ages in one or both ears. Individuals are usually not born with hyperacusis, but may develop a narrow tolerance to sound.
Individuals who suspect they may have hyperacusis should seek an evaluation by one of experts. There are no specific corrective surgical or medical treatments for hyperacusis. However, sound therapy may be used to “retrain” the auditory processing center of the brain to accept everyday sounds.
Perforated Eardrum
Traumatic causes include direct trauma such as with use of a bobby pin or Q-tip, skull fracture, or slap to the ear. Middle ear infections may lead to spontaneous rupture of the eardrum with infected or bloody drainage from the ear. In patients with chronic Eustachian tube problems, the ear drum may become progressively weakened and a perforation to occur. On some occasions, a small hole may remain in the eardrum after a previously placed pressure-equalizing tube falls out or is removed.
Most eardrum holes resulting from injury or an acute ear infection heal on their own. The chance of a perforation healing on its own depends on the size of the perforation. If the perforation does not spontaneously heal, then surgical options can be considered.
Our specialists at C/V ENT Surgical Group will advise you regarding the proper care of a hole in the eardrum.
Swimmer’s Ear/Otitis Externa
Swimmer’s ear or acute otitis externa is a painful condition resulting from inflammation, irritation, or infection of the outer ear canal. These symptoms often occur after water gets trapped in your ear, with subsequent spread of bacteria or fungal organisms. When water is trapped in the ear canal, bacteria that normally inhabit the skin and ear canal multiply, causing infection of the ear canal.
Other causes of otitis externa include:
- Contact with polluted water
- Excessive cleaning of the ear canal
- Damage to the skin of the ear canal following water irrigation to remove wax
- A cut in the skin of the ear canal
- Other skin conditions affecting the ear canal, such as eczema
Our ENT surgeons at C/V ENT Surgical Group will examine your ears, carefully clean your ear canal and typically prescribe eardrops that inhibit bacterial or fungal growth and reduce inflammation. If the ear canal is swollen shut, a wick may be placed in the canal so the antibiotic drops will enter the swollen canal more effectively. Follow-up appointments are very important to monitor improvement or worsening, to clean the ear again, and to replace the ear wick as needed. At C/V ENT Surgical Group, we have specialized equipment and expertise to effectively clean the ear canal and treat swimmer’s ear.
Tinnitus
Tinnitus may be caused by different parts of the hearing system. In the outer ear, excessive ear wax can result in tinnitus. Middle ear problems including middle ear infections may lead to tinnitus. Most subjective tinnitus associated with the hearing system originates in the inner ear. Damage and loss of the tiny sensory hair cells in the inner ear may be commonly associated with the presence of tinnitus. In certain cases, tinnitus may develop with loud noise exposure even before hearing loss. Medications can also damage inner ear hair cells and cause tinnitus. As we age, the incidence of tinnitus increases.
Tinnitus may also originate from lesions on or in the vicinity of the hearing portion of the brain. These include a variety of uncommon disorders including vestibular schwannoma (acoustic neuroma) and damage from head trauma.
Another category is pulsatile tinnitus that sounds like one’s heartbeat or pulse. Infrequently, pulsatile tinnitus may signal the presence of cardiovascular disease or a vascular tumor.
Voice and swallowing disorders among common ENT problems
Nodules, Polyps, and Cysts
A vocal cord polyp typically occurs only on one side of the vocal cord and can occur in a variety of shapes and sizes. Depending upon the nature of the polyp, it can cause a wide range of voice disturbances.
A vocal cord cyst is a firm mass of tissue contained within a membrane. As with vocal cord polyps and nodules, the size and location of vocal cord cysts affect the degree of disruption of vocal cord vibration and subsequently the severity of hoarseness or other voice problem. Surgery followed by voice therapy is the most commonly recommended treatment for vocal cord cysts that significantly alter and/or limit voice.
A reactive vocal cord lesion is a mass located opposite an existing vocal cord lesion, such as a vocal cord cyst or polyp. This type of lesion is thought to develop from trauma or repeated injury caused by the lesion on the opposite vocal cord. A reactive vocal cord lesion will usually decrease or disappear with voice rest and therapy.
Changes in vocal quality and persistent hoarseness are typically the first warning signs of a vocal cord lesion. When a vocal cord lesion is present, symptoms may increase or decrease in degree, but will persist and do not go away on their own.
Hoarseness
Causes of hoarseness include: Acute laryngitis, vocal abuse and misuse, benign vocal cord lesions (nodules, polyps, and cysts,) vocal hemorrhage, GERD/LPR, smoking, neurological disorders, vocal cord paralysis, and cancers of the airway and throat.
Otolaryngologists will obtain a thorough history of a patient’s hoarseness and general health. They will then evaluate the voice and do a complete ear, nose, and throat exam. This includes examination of the vocal folds by laryngoscopy. Laryngoscopy may be suggested by the otolaryngologist at any time during an evaluation for hoarseness, but if it persists beyond three weeks it should be evaluated and that evaluation should occur within a maximum of 3 months. The evaluation should be immediate if there is concern about a serious underlying cause is suspected.
Our specialists at C/V ENT Surgical Group which serves the greater Los Angeles and Thousand Oaks areas, will often utilize various scopes and likely video stroboscopy to determine the cause of your voice disorder and then plan a proper treatment course.
Laryngeal Surgery
Our specialists at C/V ENT Surgical Group which serves the greater Los Angeles and Thousand Oaks areas, will often utilize various scopes and likely video stroboscopy to determine the cause of your voice disorder and then plan a proper treatment course. If this treatment involves surgery then they will schedule your for a microsuspension direct laryngoscopy which is an outpatient procedure performed at a surgery center. In this short procedure a microscope and fine microsurgical instruments are utilized to treat your laryngeal problem. Most patients are able to leave within one to two hours following the procedure.
GERD and LPR
Gastroesophageal reflux disease, often referred to as GERD, occurs when acid from the stomach backs up into the esophagus. In some cases, reflux can be silent, with no heartburn.
During gastroesophageal reflux, the contents of the stomach and upper digestive tract may reflux all the way up the esophagus, and into the back of the throat and possibly the back of the nasal airway. This is known as laryngopharyngeal reflux (LPR). Adults with LPR often complain that the back of their throat has a bitter taste, a sensation of burning, throat clearing, voice changes ,or foreign body sensation. Many patients with LPR do not experience heartburn.
For proper diagnosis and treatment, our doctors at C/V Surical Group will perform a thorough examination usually including examination of the throat and pharynx with a special scope (laryngoscopy.)
Lifestyle changes a large part of the treatment of LPR. These include:
- Avoid eating and drinking two to three hours prior to bedtime
- Do not drink alcohol
- Eat small meals and slowly
- Limit caffeine, carbonated drinks, chocolate, tomato, citrus fruits, fatty and fried foods, and spicy foods.
- Weight loss
- Quit smoking
- Wear loose clothing
Swallowing Trouble
Difficulty in swallowing (dysphagia) is common among all age groups, especially the elderly. The process of swallowing has four stages:
- Oral preparation stage: Food or liquid is manipulated and chewed in preparation for swallowing.
- Oral stage: The tongue propels the food or liquid to the back of the mouth, starting the swallowing response.
- Pharyngeal stage: Begins when food or liquid is quickly passed through the pharynx and into the esophagus.
- Esophageal stage: The food or liquid passes through the esophagus and into the stomach.
Dysphagia has a number of causes. Any interruption in the swallowing process can cause difficulties. Eating slowly and chewing thoroughly can help reduce problems with swallowing. Dysphagia may be due to poor teeth, ill fitting dentures, common cold, or gastroesophageal reflux. Other causes include hypertension; diabetes; thyroid disease; stroke; progressive neurologic disorder; medications; a paralyzed or unmoving vocal cord; a tumor in the mouth, throat, or esophagus; or prior surgery or radiation therapy in the head, neck, or esophageal areas.
When dysphagia is persistent and the cause is not apparent, our surgeons at C/V Surgical Group will discuss the history of your problem and examine your mouth and throat. Often a flexible laryngoscope is placed through the nose with visualization of the back of the tongue, throat, and larynx.
Snoring and Sleep apnea surgery
Our doctors at C/V ENT Surgical Group, serving the Los Angeles and Thousand Oaks areas, are experts in the diagnosis and treatment of snoring and sleep apnea. They will start with obtaining a thorough history of your concerns and symptoms and subsequently perform a workup to diagnose the cause of your sleep disorder. Once a diagnosis is reached, whether this may be simple snoring or severe obstructive sleep apnea (OSA), they can guide you regarding which treatment options may be best to help you obtain restful sleep not only for you but also for your bed partner. These options are detailed below and they include various procedures including in-office procedures with minimal downtime to more invasive surgical procedures.
What is obstructive sleep apnea (OSA)?
Sleep apnea is a common disorder that can be very serious. In sleep apnea, your breathing stops or gets very shallow while you are sleeping. Each pause in breathing typically lasts 10 to 20 seconds or more. These pauses can occur 20 to 30 times or more an hour.
The most common type of sleep apnea is obstructive sleep apnea. During sleep, enough air cannot flow into your lungs through your mouth and nose even though you try to breathe. When this happens, the amount of oxygen in your blood may drop. Normal breaths then start again with a loud snort or choking sound.
When your sleep is upset throughout the night, you can be very sleepy during the day. With sleep apnea, your sleep is not restful because:
- These brief episodes of increased airway resistance (and breathing pauses) occur many times.
- You may have many brief drops in the oxygen levels in your blood.
- You move out of deep sleep and into light sleep several times during the night, resulting in poor sleep quality.
People with sleep apnea often have loud snoring. However, not everyone who snores has sleep apnea. Some people with sleep apnea don’t know they snore.
- Sleep apnea happens more often in people who are overweight, but even thin people can have it.
- Most people don’t know they have sleep apnea. They don’t know that they are having problems breathing while they are sleeping.
- A family member and/or bed partner may notice the signs of sleep apnea first.
Untreated sleep apnea can increase the chance of having high blood pressure and even a heart attack or stroke. Untreated sleep apnea can also increase the risk of diabetes and the risk for work-related accidents and driving accidents.
What causes sleep apnea?
Sleep apnea happens when enough air cannot move into your lungs while you are sleeping. When you are awake, and normally during sleep, your throat muscles keep your throat open and air flows into your lungs. In obstructive sleep apnea (OSA), however, the throat briefly collapses, causing pauses in your breathing. With pauses in breathing, the oxygen level in your blood may drop. This happens if the following conditions occur:
- Your throat muscles and tongue relax more than is normal.
- Your tonsils and adenoids are large.
- Your nose is obstructed due to a deviated septum, large turbinates or nasal polyps.
- You are overweight.
- The extra soft tissue in your throat makes it harder to keep the throat area open.
- The shape of your head and neck (bony structure) results in somewhat smaller airway size in the mouth and throat area.
- You have a very floppy palate with a thick or long uvula.
- You have a very large base of tongue that flops back and blocks your breathing.
With these areas in your nose and throat being partly blocked during sleep, enough air cannot flow into your lungs, even though your efforts to breathe continue. Your breathing may become hard and noisy and may even stop for short periods of time (apneas).
Another rare type of sleep apnea, termed central sleep apnea, happens when the area of your brain that controls your breathing doesn’t send the correct signals to the breathing muscles. Then there is no effort to breathe at all for brief periods. Snoring does not typically occur in central apnea and is not treated by our surgeons.
Who is at risk for obstructive sleep apnea (OSA)?
Anyone can have obstructive sleep apnea.
It is estimated that more than 12 million Americans have obstructive sleep apnea. More than half the people who have sleep apnea are overweight, and most snore heavily.
Sleep apnea is more common in men. One out of 25 middle-aged men and 1 out of 50 middle-aged women have sleep apnea that causes them to be very sleepy during the day. Sleep apnea is more common in African Americans, Hispanics, and Pacific Islanders than in Caucasians. If someone in your family has sleep apnea, you are more likely to develop it than someone without a family history of the condition.
Adults who are most likely to have sleep apnea:
- Snore loudly.
- Are overweight.
- Have high blood pressure.
- Have a decreased size of the airways in their nose, throat, or mouth. This can be caused by the shape of these structures or by medical conditions causing congestion in these areas, such as hay fever or other allergies.
- Have a family history of sleep apnea.
Obstructive sleep apnea can also occur in children who snore. If your child snores, you should discuss it with our physicians.
What are the symptoms of obstructive sleep apnea (OSA)?
The most common signs of sleep apnea are:
- Loud snoring
- Choking or gasping during sleep
- Fighting sleepiness during the day (even at work or while driving)
Your family members may notice the symptoms before you do. Otherwise, you will likely not be aware that you have problems breathing while you are asleep.
Others signs of sleep apnea may include:
- Morning headaches
- Memory or learning problems
- Feeling irritable
- Not being able to concentrate on your work
- Mood swings or personality changes perhaps feeling depressed
- Dry throat when you wake up
- Frequent urination at night
How is obstructive sleep apnea (OSA) diagnosed?
Your doctors will do a physical exam, take a medical history that includes asking you questions about how you sleep and how you function during the day and have you fill out a detailed questionnaire that will risk-stratify you in relation to your snoring and sleep apnea. As part of the exam, your doctor will check your mouth, nose, and throat to determine areas of obstruction. For example, a deviated spetum, large turbinates, enlarged tonsils, a long or thick uvula (the tissue that hangs down in the middle in the back of your throat), a floppy soft palate or a large base of tongue. Your doctor may order a sleep recording if your symptoms are severe enough based on your history, exam and questionnaire results to grade your sleep apnea into mild, moderate or severe types.
What are the treatment options for snoring and obstructive sleep apnea?
Continuous Positive Airway Pressure (CPAP):
Continuous positive airway pressure (CPAP) is the most common treatment for moderate to severe sleep apnea and is the gold standard for treatment, however many people cannot tolerate use of this cumbersome mask and machine. For this treatment, you wear a mask over your nose during sleep. The mask blows air into your throat at a pressure level that is right for you. The increased airway pressure keeps the throat open while you sleep.
If you are one of the many who cannot tolerate CPAP for one reason or another and you have mild to moderate sleep apnea you may be a candidate for one of the surgical treatment options the physicians at C/V ENT Surgical Group in Los Angeles utilize listed below, which include in-office procedures.
Pillar Implant Procedure
Once in place, the inserts add structural support to the soft palate. Over time, the body’s natural tissue response to the inserts (which are made of nothing more than suture material that is used in everyday surgery) increases the structural integrity of the soft palate. This procedure is performed in the office under local anesthesia and usually takes about 30 minutes. One can return to normal eating and function the same day. Results, however are not seen until 2-4 months after the procedure when the palate has stiffened due to the normal scarring process.
A study performed in Norway indicated that the procedure is successful (70%) in terms of bed-partner satisfaction (Nordgard, 2006). The cure rate for sleep apnea depends on the severity of the preoperative level of sleep apnea. However studies have shown it is 80-90% effective as a treatment for snoring.
Our surgeons at C/V ENT Surgical Group, which serves the Los Angeles and Thousand Oaks areas, are now utilizing this procedure with great results. Sometimes they perform this procedure in combination with a coblation assisted uvulectomy to target both the anterior and posterior soft palate in patients with a large uvula. Note that laser uvulectomy, if performed, does add a moderate amount of post-procedural pain and discomfort to the in-office procedure.
The pillar implant procedure was recently highlighted on “The Doctors” and can be seen here:
Laser Assisted Uvulopalatoplasty (LAUP)
Coblation
Tonsillectomy and Adenoidectomy
Uvulopalatopharyngoplasty (UP3/UPPP)
The hardest part is not the surgery itself, but the recovery from this procedure. There is significant pain for 7-15 days, as the area in the back of the throat heals, requiring pain medication regularly and a liquid or soft diet for that period. This procedure is at times combined with tongue base reduction surgery when indicated. Our surgeons perform uvulopalatopharyngoplasty (UP3/UPPP) in patients with moderate to severe obstructive sleep apnea that are noted on exam to be good candidates and have failed CPAP treatment.
Tongue Base Reduction
Septoplasty
Submucous Resection of Inferior Turbinates
Thyroid and parathyroid surgery
Our surgeons are renowned head and neck surgeons at C/V ENT Surgical group in Los Angeles and Thousand Oaks, represent a select number of surgeons in the country that routinely perform minimally invasive thyroidectomy as well as minimally invasive parathyroidectomy in select patients after careful workup. The standard approach for these lesions has and continues to be in many centers around the country a standard 4-5 inch collar incision in the lower neck. However, the physicians here utilize small 1 to 1.5 inch incisions in the lower neck hidden in a usual skin crease to perform these delicate procedures with the aid of either endoscopes or eye-loop magnification. This surgery has only come to fruition over the past few years and only certain surgeons in the country are qualified or have completed advance training to be able to perform these delicate and complicated surgeries. As such the surgeons at C/V now spend a part of their time teaching others in the field these skillfully demanding procedures. Furthermore Dr. Cohen is now Director of the Minimally Invasive Thyroid/Parathyroid Surgery program and West Hills Medical Center, the only center in the San Fernando and Conejo Valleys.
Minimally Invasive Thyroid Surgery
Minimally Invasive Parathyroid Surgery
Hemithyroidectomy
Total Thyroidectomy
Thyroid Cancer Surgery
Thyroid Goiter Surgery
Parathyroid Exploration
Central Neck Compartment Dissection
Lateral Neck Compartment Dissection
Head and Neck surgery
The head and neck region houses some of the most complex anatomy in the human body that is involved in all of our daily activities. This region includes all structures from the skull base to the clavicle. For example the key organs that allow us to hear, see, communicate, breathe, swallow, smell and taste are all located in this region. As such, the head and neck surgeon needs to have an extensive knowledge of the anatomy and function of various structures in this region but also to have the skill and training to treat these disorders while cognizant of cosmesis and function.
That is why the physicians at C/V ENT Surgical Group have extensive head and neck surgical training and when treating complex issues in this area they are always mindful of form and function in their patients. As such they represent a select few head and neck surgeons in the country that utilize minimally invasive techniques in the treatment of various head and neck disorders and tumors.
Excision of Benign Tumors
Various benign tumors or masses can arise in the head and neck region ranging from superficial skin lesions such as cysts or skin tags to deeper more infiltrating masses like lipomas and branchial cleft cysts. These tumors can often times be close to various critical vessels and nerves and as such require careful removal by top head and neck surgeons. Our surgeons at C/V Surgical Group in West Hills go to great lengths to formulate and execute an appropriate surgical plan to remove these tumors with minimal risk to any critical structures. They also always strive to make the smallest incision possible that can provide safe removal with minimal cosmetic deformity.
Excision of Malignant Tumors
Malignant tumors do arise in the head and neck region and depending on the pathology various surgical procedures are indicated ranging from simple biopsy to radical excision of these tumors with adequate margins. Our renowned head and neck surgeons have extensive experience with the proper workup and treatment of these various malignancies and will guide you through every step of the process in order to provide you with the best chance for cure. Function and cosmesis are paramount in their decision-making in the management of these malignancies. The office is located in the West Hills/Calabasas region of the San Fernando Valley but serves the greater Los Angeles and Thousand Oaks area and often times people will fly in for their expertise.
Excision of Skin Cancers
Skin cancer is a disease in which cancer (malignant) cells are found in the outer layers of your skin. There are several types of cancer that originate in the skin. The most common types are basal cell carcinoma (70 percent of all skin cancers) and squamous cell carcinoma (20 percent). These types are classified as nonmelanoma skin cancer. Melanoma (five percent of all skin cancers) is the third type of skin cancer. It is less common than basal cell or squamous cell carcinoma, but potentially much more serious. Other types of skin cancer are rare.
When skin cancers arise on you face or neck regions you should trust your face only to a facial plastic surgeon not only to resect the cancer but also for reconstruction of the defect so that you wont be left with a significant cosmetic deformity. Our specialists at C/V ENT Surgical Group, which serves the greater Los Angeles area, have particular experience in the management of skin cancers and melanoma of the face and neck region. Also at times these cancers may have predilection for local metastasis to lymph nodes in the region and they will address the metastatic deposits adequately with parotidectomy or neck dissection. In the treatment of melanoma often sentinel lymph node biopsy is also employed for proper staging.
Head and Neck Cancer Surgery
More than 55,000 Americans develop head and neck cancer annually. As many as 90 percent of head and neck cancers arise after prolonged exposure to specific factors. Use of tobacco (cigarettes, cigars, chewing tobacco, or snuff) and alcoholic beverages are closely linked with cancers of the mouth, throat, voice box, and tongue. If you have these risk factors and notice a lump or a mass that is not resolving after 2-3 weeks in the nose, throat, mouth, face or neck regions then evaluation by a head and neck surgeon is prudent for further workup of this mass. This workup may include imaging studies such as ultrasound, CT or MRI as well as biopsy. Based on the workup, then a discussion will be had between you and one of our renowned surgeons, at C/V ENT Surgical Group in Los Angeles, to decide the best course of treatment. This decision is made after discussion of all the options available including radiation therapy, chemotherapy and surgery.
Neck Dissection
Neck Mass Excision
Neck masses can present often times in both the adult and pediatric population. If a mass in the neck is present for more than 2 to 3 weeks and is larger than the size of your fingertip, then an evaluation by a Head & Neck Surgeon is warranted. These masses are often times benign in nature but an evaluation is always warranted. This evaluation may be followed by an imaging study such as an ultrasound, CT or MRI to determine the exact size and location of the neck mass. If the imaging study shows a mass that is greater than a certain size, then further procedures such as surgical excision of the mass or needle biopsy may be indicated. If surgery is warranted, then our surgeons in West Hills/Calabasas, have extensive experience in the proper excision of these neck masses while being mindful of function and cosmesis. Remember that the neck houses many critical nerve and vascular structures and only a head and neck surgeon has the proper training to adequately minimize trauma these structures while successfully removing the mass.
Parotid Surgery
The parotid gland is one of our major salivary glands and resides on the side of the face just in front of the ear. The gland is divided into a superficial lobe and deep lobe by the facial nerve. The facial nerve is a major cranial nerve that comes out of the skull base from the brain just below and in front of our ear lobe. It divides into multiple branches after exiting the skull base and controls all of our facial muscles that make us raise our eyebrows, close our eyes, pucker our lips, and smile. Often times tumors develop in the parotid gland, these are usually benign in nature (80%) but may also be malignant (20%) at times. Signs that a parotid tumor may be malignant are facial weakness or pain upon presentation. When a parotid mass is identified then an evaluation by a board-certified head and neck surgeon is warranted for proper workup and then definitive treatment. This work-up often includes an imaging study, usually an MRI for better delineation of soft tissue anatomy, and a fine needle aspiration of the mass. Once this is complete then surgery is planned.
Parotid surgery is a very delicate and skillfully demanding procedure where the tumor needs to be removed in it’s entirety while preserving the facial nerve and it’s various branches. As such you will want to have this procedure performed by a surgeon who does more than 10-20 of these procedures annually. Our board certified head and neck surgeons routinely perform parotid surgery in Los Angeles and Thousand Oaks to remove benign and malignant parotid masses. They are very mindful of cosmesis during this procedure and often times will utilize a hidden facelift or modified facelift incision to remove the tumor. In many patients they utilize a minimally invasive facelift incision for removal of the parotid mass. They are also one of a handful of surgeons who routinely use intraoperative facial nerve monitoring to monitor the nerve during dissection of the tumor so as to minimize injury to the nerve. Lastly, our surgeons with their extensive facial plastics experience, will often utilize a muscle flap to cover the defect after a parotidectomy so that you are not left with a large and hideous indentation on the side of your face.
Salivary Gland Surgery
The major salivary glands are the parotid glands, submandibular glands and the sublingual glands. There also hundreds of minor salivary glands in our mouths along the lips, tongue, inner cheeks and palate that produce saliva. Pathology can arise in any of these glands in the forms of cysts, stones, infection/inflammation and tumors (benign or malignant). If any of these problems arise then evaluation and treatment by a head and neck surgeon is critical. Simple in-office procedure such as stone removal or duct dilation may be all that is necessary to treat the problem. However if a mass is noted in these glands then a workup will be indicated including an MRI and fine needle aspiration biopsy. Once this is completed then often surgery is required to properly remove the mass in it’s entirety while sparing critical nearby structures like important nerves. Our renowned head and neck surgeons at C/V ENT Surgical Group in Calabasas, are experts in the medical and surgical treatment of various salivary gland disorders so you can rest assured in their hands.
Tongue and Oral Cavity Surgery
The oral cavity includes the lips, tongue, palate, floor of mouth, tonsils and inner cheek linings (aka = buccal mucosa). The tongue is divided into an anterior (front) 2/3 and posterior (back) 1/3. Various pathology in the forms of cysts, ulcers, infection, inflammation and tumors can arise in these areas. If any of these problems does not resolve after 2-3 weeks then evaluation by an ear, nose and throat surgeon is prudent. The board-certified surgeons at C/V ENT Surgical Group in the San Fernando Valley are well-trained in order to diagnose and treat these problems accurately.
Reconstructive Head and Neck Surgery
Our renowned head & neck surgeons as well as facial plastic surgeons at C/V ENT Surgical Group which serves the greater Los Angeles and Thousand Oaks areas, utilize their combined experience daily to not only remove various masses and tumors in the head and neck region but also to reconstruct any defects that may be left behind to minimize any cosmetic deformity that the patient may have to endure. Especially when large skin cancers have to be removed in these critical areas, various small and large neighboring skin flaps or distant skin grafts may have to be utilized to adequately cover the defects in a cosmetically acceptable fashion.
